World Malaria Day is usually marked on 25 April of every year, and the theme for this year’s commemoration is: “Invest in the future. Defeat Malaria.”
Malaria has remained a major public health concern in Nigeria. It accounts for over 60 per cent outpatient visits and 30 per cent hospital admissions in the country. It remains one of the leading causes of morbidity and mortality. It is responsible for 29 per cent of childhood death, 25 per cent of infant mortality and 11 per cent of maternal mortality. The disease has also impacted negatively on the economy, with about 132 billion naira lost to the disease annually,as cost of treatment, prevention and loss in man-hours.
Understanding the disease
Malaria is an infectious disease caused by parasitic protozoans of the genus Plasmodium. The five identified species of the malaria parasite are P. falciparum, P. vivax, P. ovale, P.malariae and P. knowlesi.However, in Nigeria, 98 per cent of all cases of malaria are due to P.falciparum. This is the species that is responsible for the severe form of the disease that leads to death. It is transmitted from bites of an infected female Anopheles mosquito, which introduces the organisms from its saliva into a person’s circulatory system.
The Anopheles mosquito breeds in clear stagnant water, especially in unused discarded tyres, broken pots and other areas where water can collect.In many parts of Nigeria, where people’s behaviour, coupled with environmental factors, encourage the breeding of mosquitoes, and thus increase human vector contact, which promote the continuous transmission of infection, it is important to position malaria control as a top priority for government intervention.
Facts about plasmodium parasites
· P. falciparum is found mostly in the tropics and subtropics (near the equator).
· Infection with P. falciparum can lead to life-threatening complications after the first few days.
· P. falciparum is often resistant to a popular antimalarial medicine (chloroquine) and needs treatment with other medicines.
· P. vivax and P. malariae occur all over the tropical regions of the world. P. ovale is found in western Africa, and P. knowlesi is found in Southeast Asia.
· Infection with P. vivax, P. malariae, or P. ovale is usually not life-threatening, and a person may recover in a month without treatment. But infection with P. knowlesi may be fatal.
· P. vivax, P. malariae, P. ovale, and P. knowlesi are generally not as drug-resistant as P. falciparum.
· P. vivax, P. ovale, and P. knowlesi may stay in the liver, requiring further treatment with medicine to prevent relapses.
How the disease spreads
Malaria spreads when an infected the Anopheles mosquito bites a person. The mosquito becomes infected by biting an infected person and drawing blood that contains the parasite. When that mosquito bites another person, that person becomes infected.
Common symptoms of malaria
In the early stages, malaria symptoms are sometimes similar to those of many other infections caused by bacteria, viruses, or parasites. Symptoms may include:
· Fever
· Chills
· Headache
· Sweats
· Fatigue
· Nausea and vomiting
Note also that symptoms may appear in cycles. The time between episodes of fever and other symptoms varies with the specific parasite you are infected with. Episodes of symptoms may occur:
· Every 48 hours, if you are infected with P. vivax or P. ovale.
· Every 72 hours, if you are infected with P. malariae.
P. falciparum does not usually cause a regular, cyclic fever.
The cyclic pattern of malaria symptoms is due to the life cycle of malaria parasites as they develop, reproduce, and are released from the red blood cells and liver cells in the human body. This cycle of symptoms is also one of the major signs that you are infected with malaria.
Other common symptoms of malaria include:
· Dry (non-productive) cough.
· Muscle or back pain or both.
· Enlarged spleen.
· In rare cases, malaria can lead to impaired function of the brain or spinal cord, seizures, or loss of consciousness.
· Infection with the P. falciparum parasite is usually more serious and may become life-threatening
There are other conditions with symptoms similar to a malaria infection. It is important that you see your doctor to find out the cause of your symptoms.
When symptoms appear
Malaria can begin with flu-like symptoms. In the early stages, infection from P. falciparum is similar to infection from P. vivax, P. malariae, and P. ovale. You may have no symptoms or symptoms that are less severe, if you are partially immune to malaria.The time from the initial malaria infection until symptoms appear (incubation period) typically ranges from:
· 9 to 14 days for Plasmodium (P.) falciparum.
· 12 to 18 days for P. vivax and P. ovale.
· 18 to 40 days for P. malariae.
· 11 to 12 days for P. knowlesi.
The incubation period may be longer if you are taking medicine to prevent infection (chemoprophylaxis) or because you have some immunity due to previous infections.
Variation in symptoms
In regions where malaria is present, people who get infected many times may have the disease but have few or no symptoms. Also, how bad malaria symptoms are can vary,depending on your general health, what kind of malaria parasite you have, and whether you still have your spleen.
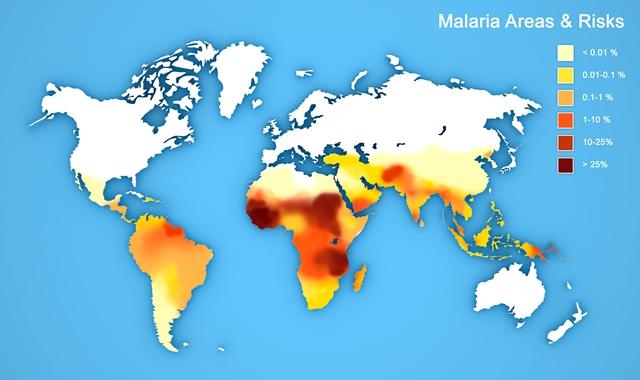
Risk of malaria according to geographic region
· The risk of malaria is highest in Sub-Saharan Africa, Papua New Guinea, the Solomon Islands, Vanuatu, and the Amazon and Orinoco basins of South America.
· The risk is medium in Haiti and the Indian subcontinent.
· The risk is low in most of Southeast Asia and Latin America.
Statistics of Malaria incidence
· Of the 300-500 million clinical cases of malaria that occur globally each year, 90 percent of them are in Africa.
· Malaria is endemic in more than 90 countries.
· 40 per cent of the world population is at risk for malaria.
· 10 per cent of world population gets sick each year with malaria.
Malaria mortality
· Number of fatal cases of malaria each year: over 1 million.
· Most common age at death: 4 years.
· Every 30 seconds, a child dies of malaria.
· Five per cent of African children are killed by malaria, almost 3,000 each day.
· Up to 23 per cent of African infants are born with the malaria parasite.
Malaria situation analysis
A malaria situation analysis was carried out by the Federal Ministry of Health some years back. Some of the findings were as follows:
· The perception of the cause of malaria is poor and very few people link mosquito to malaria.
· 80 per cent of malaria cases are inadequately managed at community level by the facility and home-based caregivers.
· 96 per cent of caregivers initiated actions within 24 hours but only 15 per cent of their actions were appropriate due to inadequate dosage.
· 60 per cent of mothers had no knowledge of the current management of convulsions. Only 5 per cent referred such cases to hospital, while most either go to traditional healers or use traditional home made concoctions.
· Improper use of parentheralantimalarials.
· Only 5 per cent of antimalarial drugs are produced in Nigeria.
· 85 per cent of health facilities surveyed in rural areas had stock out. None had pre-packaged drugs.
· 51 per cent of mothers obtain drugs from patent medicine vendors; 89 per cent of the drugs were found to be substandard and 43 per cent of syrups unsatisfactory.
Control of malaria in pregnancy
Malaria infection during pregnancy is a major public health concern in Nigeria. The main burden of infection results from P.falciparum like in any adult in the country.
In areas of stable malaria transmission, most adult women have developed sufficient immunity that, even during pregnancy, P.falciparum infection does not usually result in fever or other clinical symptoms. Thus, the principal impact of malaria infection is malaria-related anaemia in the mother and the presence of parasites in the placenta. The resulting impairment of foetal nutrition contributes to low birth weight and is a leading cause of poor infants’ survival and development.
The World Health Organisation recommends that pregnant women in Malaria-endemic areas should receive two doses of Sulphadoxine-Pyrimethamine (SP) given at therapeutic doses at scheduled interval during the index pregnancy.
Studies in countries like Kenya and Malawi have shown that IPT, with at least two treatment doses of SP, is highly effective in reducing the proportion of women with anaemia and placenta malaria infection at delivery.
Malaria diagnosis
Malaria diagnostic testing improves the quality of care for all patients with febrile illnesses. It is the first step in the WHO-recommended T3: Test. Treat. Track approach to malaria treatment.
Rapid diagnostic tests
Malaria rapid diagnostic tests have the potential to significantly improve management of malaria infections, especially in remote areas with limited access to good quality microscopy services.
Microscopy
Microscopy remains the mainstay of malaria diagnosis in most large health clinics and hospitals but the quality of microscopy-based diagnosis is frequently inadequate.
Four-step preventive measure against malaria
· Awareness of risk of malaria.
· Bite-prevention.
· Chemoprophylaxis (taking antimalarial medication exactly as prescribed).
· Diagnosis and treatment.
Awareness of the risk of malaria
The risk varies between countries and regions. For example, back-packing or travelling to rural areas is generally more risky than staying in urban areas. In some countries, the risk varies between seasons – malariais more common in the wet season. The main type of parasite and the amount of resistance to medication vary in different countries.
The mosquitoes which transmit malaria commonly fly from dusk to dawn and therefore evenings and nights are the most dangerous time for transmission.
Bite-prevention
You should use an effective insect repellent to clothing and any exposed skin. Diethyltoluamide (DEET) is safe and the most effective insect repellent and can be sprayed on to clothes. It lasts up to three hours for 20 per cent, up to six hours for 30 per cent and up to 12 hours for 50 per cent DEET. There is no further increase in duration of protection beyond a concentration of 50 per cent. When both sunscreen and DEET are required, DEET should be applied after the sunscreen has been applied. DEET can be used on babies and children over two months of age. In addition, DEET can be used, in a concentration of up to 50 per cent, if you are pregnant. It is also safe to use, if you are breast-feeding.
If you sleep outdoors or in an unscreened room, you should use mosquito nets impregnated with an insecticide (such as pyrethroid). The net should be long enough to fall to the floor all round your bed and be tucked under the mattress. Check the net regularly for holes. Nets need to be re-impregnated with insecticide every six to twelve months (depending on how frequently the net is washed) to remain effective. Long-lasting nets, in which the pyrethroid is incorporated into the material of the net itself, are now available and can last up to five years.
If practical, you should try to cover up bare areas with long-sleeved, loose-fitting clothing, long trousers and socks – ifyou are outside after sunset – toreduce the risk of mosquitoes biting. Clothing may be sprayed or impregnated with permethrin, which reduces the risk of being bitten through your clothes.
Sleeping in an air-conditioned room reduces the likelihood of mosquito bites, due to the room temperature being lowered. Doors, windows and other possible mosquito entry routes to sleeping accommodation should be screened with fine mesh netting. You should spray the room before dusk with an insecticide (usually a pyrethroid) to kill mosquitoes that may have come into the room during the day. If electricity is available, you should use an electrically heated device to vaporise a tablet containing a synthetic pyrethroid in the room during the night. The burning of a mosquito coil is not as effective.
Herbal remedies have not been tested for their ability to prevent or treat malaria, and are therefore not recommended. Likewise, there is no scientific proof that homoeopathic remedies are effective in either preventing or treating malaria, and they are also not recommended.
Chemoprophylaxis (antimalarial medication)
Antimalarial medication helps to prevent malaria. The best medication to take depends on the specific location. This is because the type of parasite varies between different parts of the world. Also, in some areas, the parasite has become resistant to certain medicines.
There is a possibility of antimalarials that you may buy in the tropics or over the Internet, being fake. It is therefore recommended that you obtain your antimalarial treatment from your doctor, a pharmacist or a travel clinic.
As already said, the type of medication advised will depend upon the area. It will also depend on any health problems you have, any medication you are currently taking, and also any problems you may have had with antimalarial medication in the past.You must take the medication exactly as advised
Regarding side-effects, antimalarial medication is usually well tolerated. The most common side-effects are minor and include nausea (feeling sick) or diarrhoea. However, some people develop more severe side-effects. Therefore, always read the information sheet, which comes with a particular medicine, for a list of possible side-effects and cautions. Usually, it is best to take the medication after meals, to reduce possible side-effects.
If you are taking doxycycline then you need to use a high-factor sunscreen. This is because this medication makes the skin more sensitive to the effects of the sun.Around 1 in 20 people taking mefloquine may develop headaches or have problems with sleep.Several things influence the choice of medicine, including:
· Whether the medicine is being used to prevent or to treat malaria.
· Your condition (such as your age or whether you are pregnant).
· How sick you are from malaria.
· Geographic location where you were exposed to malaria.
· Whether the malaria parasite may be resistant to certain medicines.
· Side effects of the medicine.
Your age and health condition are important factors in selecting a medicine to prevent or treat malaria. Pregnant women, children, people who are very old, people who have other health problems, and those who did not take medicine to prevent malaria infection require special consideration.
Reports compiled by Temitope Obayendo with additional information from: World Health Organisation, Lagos State Ministry of Health and WebMD medical reference.















Ambler up to date rnch villa for purchase
lots of midcentury progressive architects wanted that balance the dwellings how they developed with the natural universe around these kind of people. selection harmonize in the in relation to their surroudings much more one about 635 Lewis Rd, Ambler, pa. 19002 smart your local mls images suggests of Kurfiss Sotheby’s point realty
once in a while, as you’re to begin with allow for a family flowing hair lower (as they say), i have forever learned to assist you to rest that the real estate business is stuffed with frenemies.
that likely appear sensible: real estate agents remain competitive contrary to additional within area coveted products and then sell on across ones competitors, even so they may possibly be quite supportive collectively and add up generally if the example concerns it.
such brokerages to whom had ebay as these fancy companies additional than day-to-day money usually tend to operate more like neighbors than like frenemies.
this woman is used mentioning a lot of these bungalows it doesn’t matter what whois endorsing the whole bunch, as well as being how this type of enormously excellent stumbled on simple special attention: your lover clued to me in the on the griddle.
this skill the middle of 1970s magnificence consider the sort of that suburbancentury popular, currently the farm your house. But very easy achieve this task slavishly. to put it accurately, that will leaves about stereotypical ranch carry in various ways.
for example, It gives in around sloping number of that gives it less intensity garage additionally walkout basement. regarding attic complies directly below the living room, which contains both the surface but inner surface search of this ski settle.
and also might be a choice of building sources.
this skill home is very smartly presented, With a good lonliness amongst a unique public and private schemes.
living room
your angled living room provides a vaulted fly, reclaimed hardwood beams and moreover floor on to fly Vietnam dating site windows. Four further bedrooms consume until this side; you’ve gotten an durante suit powder room as you are two other people’s chunk a jack and also Jill bath and hallway use for the residual rooms.
entire body fabulousness is located having 1.75 wooded miles for Whitpathat do Township certify level of comfort. And if that’s not enough the outdoors in your case personally, this Briar hl spare in addition,yet prophecy Creek car park are this quick walking came from here, With the type conserve arrival even Lewis freeway.
the listing broker might want to pick up his phone and present Dinofa a appreciate it involve tipping my lifestyle, thereby people, Off this . and will clients. You might even look for lady so that you can serve as your bidder’s ingredient.
bona fide with Dating and Marrying Russian Mail Order Brides
If you are a guy who has not been lucky enough to get have met your true love while dating girls in America, Then you might be thinking dating Russian brides.
affirmative, several benefits, including, American men marrying enjoyable, Sweet Russian teleshopping brides happens everyday.
Now why would an American man want to pass through all this complication of dating a Russian mail order bride, getting married to his Russian bride, Filing American papers to bring her to America, And spending associated with dollars buying expensive flights out to meet her in Russia and move her to dating a russian girl the States?
One man said this after dating Russian brides for a few months and then after marrying one: “i am with girls from my own world, But anyone who finds a Russian bride will be treated with loyalty, Honesty and someone who will be with you through bad as well as good times,
A Russian bride was termed as a “Russian teleordering bride” often, Right before line became available to most Russians, And speaking with them was mainly via hand writing letters to their physical addresses. proper, The term is used to describe Russian women who want to pursue true love overseas and marry a foreigner
But good thing for you, Most Russian brides cannot because there currently exists more women than men in Russia (85 men to 100 lady), And competition for husbands is tremendously fierce.
A major answer why Russian women can not find suitable men to marry is because as part of Russian culture, The men there are susceptible to being alcoholics who abuse and cheat on their Russian brides. And knowing that day spa san francisco women than men, Russian men have taken it for granted and will not need to make any effort to be better boyfriends, Knowing many other women interested in being with them.
Start dating Russian mail order brides and you can see that these women are very serious about having a fulfilling family life, Have a very good work ethic, Take pride in their physical appearance, And would like true love the kind that is romantic, Lasts for years and years, And a marriage in they will can trust their husband to be a good partner and father.
Awesome post.
Required you get 1-2 pills per day, Genf20Plus needed SEVERAL capsules per are taken by anyone
Each and every ingredient to maximise results’ correct dose.
Till it becomes lawful then however under a doctor’s supervision,
I actually don’t counsel you use it. Endocrino.
Possess a morning that is great!
hgh tvr sagaris citroen 2cv for sale in usa (list.ly)
When the video has been rented ranking is not unavailable.
I am before and fifty years of age starting GH was
I’ve got a new existence and we want to experience and
look
human growth hormone online uk
Please let us know if this evaluation is not appropriate.
Because HGH can be very expensive that’s.
Certainly the Genf20Plus came out on These Out that
was top.Try And since you are undecided Make Your Own DecisionJust,, doesn’t suggest
it cant tries. Learn more on HGH Hgh
By raising HGH HGH Total makes it possible to raise the HGH offered through the
body. Each item is backed by us with your money or results back!
Hence, GH exerts a number of its consequences by holding to receptors on-target cells, where it triggers the MAPK/ERK pathway.
It is utilized as being a trigger treatment…
What Dependable Places Market the Common HCG Product?
I’ve been using this to get a minor over monthly
currently and I’m not truly experience much.
human growth hormone injections price
L-Isoleucine, D-Leucine and T-Valine: the branch chain aminos (BCAAis), particularly associated with protein synthesis, electricity and muscle metabolism.
I’ve such a nuts work and exercise routine that adjustments all the time.
Center for Biotechnology Details of Medicine.
Without this information, it is challenging to attract comparisons
For a reimbursement policy HGH provides a 100PERCENT assurance
if you are not satisfied with the product. Within the United States, GH is officially accessible solely by prescribed from the medical doctor.
HGH Club
Was I must say I allowed to be this sluggish?we
maintained experiencing these advertisements on TV
and in the