Unintended pregnancies are pregnancies that are unplanned or unwanted at the time of conception. It is estimated that as many as 41 percent of the 208 million worldwide pregnancies in 2008 were unintended. These pregnancies can be associated with increased risk for both the mother and infant; lack of preconception planning and prenatal care can lead to behaviors linked to birth defects, including low levels of folic acid and maternal alcohol use.
Emergency contraception is birth control used after unprotected sexual intercourse, either due to suspected contraception failure (e.g. broken condom) or lack of contraception. It offers women a last chance to prevent an unintended pregnancy. There are two main categories of emergency contraception, emergency contraceptive pills and intrauterine devices.
Emergency contraceptive pills
There are two main categories of emergency contraceptive pills, progestin only pills containing levonorgestrel (marketed as Plan B and Next Choice) and progesterone antagonists containing ulipristal acetate (marketed as ella/ellaOne). These are collectively referred to as the ‘morning after pill’. Both categories most likely work by preventing or delaying ovulation (the release of the egg from the ovary). These pills are effective when taken anywhere from immediately after intercourse to approximately 5 days after intercourse, although the recommendation is typically to take them as soon as possible or within 72 hours. Side effects are generally mild, and may include changes in menstrual bleeding, headache and nausea. These pills are now available in over 140 countries, and available over the counter in 60 countries.
Intrauterine devices
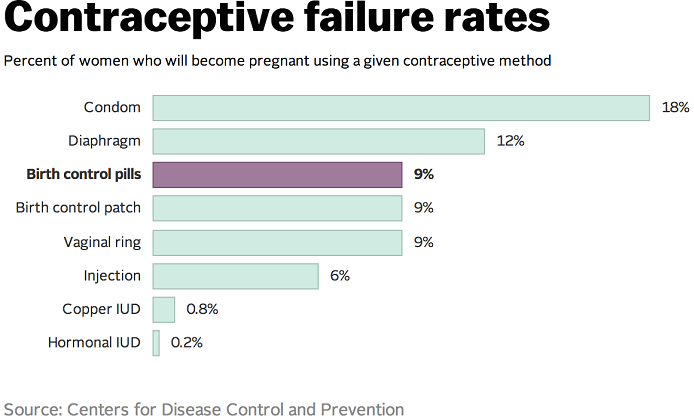
Intrauterine devices (IUDs) are small T-shaped frames that sit within the endometrial cavity, the central portion of the uterus. The IUD is inserted by a doctor or trained nurse in an office setting; this takes only a few minutes. The type of IUD approved for emergency contraception is a copper IUD. Copper IUDs prevent pregnancy in two ways. First, the copper is toxic to the sperm, and induces the uterus and fallopian tubes to release a fluid hostile to sperm. Second, the IUD changes the walls of the uterus, making it impossible for a fertilized egg to implant in the wall. Most protocols allow insertion of an IUD up to 5 days after unprotected intercourse. Side effects can include changes in menstrual bleeding.
Intrauterine devices are the most effective form of emergency contraception
IUDs are widely used worldwide for contraception, more so in Europe and Asia than in the United States. However, their use and availability for emergency contraception varies widely. Researchers from Princeton University recently examined data from six countries stretching over a 35 year time period from 1979 to 2011. Their results, published in the journal Human Reproduction, suggest that IUDs are by far the most effective method of emergency contraception, with only approximately 1 pregnancy for every 1000 insertions, or a failure rate of approximately 0.1 percent. By contrast, morning after pills have a failure rate of 1 percent to 3 percent, ten to thirty times higher. Furthermore, emergency contraceptive pills are less effective in overweight and obese patients, probably due to the slower absorption of hormones. Overweight women have an approximate 1.5 times greater pregnancy risk, with obese women having a 3 times greater pregnancy risk.
IUDs can also be left in place for up to ten years, providing long-term birth control and obviating the need for future emergency contraception. However, barriers exist to the more widespread use of IUDs for emergency contraception. One such barrier is convenience: emergency contraception pills are available over the counter in many countries, while IUD insertion requires at least one and often two office visits. A second barrier is price: emergency contraceptive pills typically cost between $10 and $70 USD, while IUD insertion costs $500 USD and up. However, if the IUD is left in place for ongoing contraception, it becomes a cost effective means of emergency contraception in as little as four months after insertion. Finally, lack of both physician and patient education means that many women seeking emergency contraception never hear about or ask about IUDs.
The researchers hope that the conclusions from this new study will help to dispel some of this lack of awareness. They urge providers to consider recommending IUDs for emergency contraception, and to make the process easier for patients by offering same day insertion.
http://www.healthguidance.org













