“As of February 6, there have been 365 confirmed cases of Lassa fever and 47 deaths in 23 Nigerian states.”
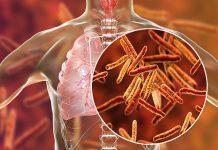
Lassa fever, also known as Lassa Haemorrhagic Fever (LHF) is a viral infection caused by the Lassa virus.
The Lassa virus has its roots in Nigeria and it is named after the town in Bornu where the first case was identified in 1969. It affects 10 out of the 18 countries in West Africa, where it majorly occurs.
In some areas of Sierra Leone and Liberia, it is known that 10-16 per cent of people are usually admitted to the hospital every year due to Lassa fever outbreak.
Approximately, 300,000 – 500,000 cases are reported annually which has led to 5000 deaths. Among casualties of Lassa fever ar medical professionals and other volunteer healthcare workers. Aniru Conteh, a renowned Sierra Leonean Lassa fever expert whose works are still relevant today was among the earliest medical professionals to lose their lives while tackling the virus.
Unlike the coronavirus virus which affects mostly the elderly and immuno-compromised individuals, Lassa fever has no clear-cut preference for any age-group. Available data shows that the most affected age group is 11-40 years. This does not mean that people outside this age group are not at risk of getting infected.
Spread
“Within just 4 weeks, Lassa fever spread to 60 local governments, 19 states including Abuja.”
Lassa fever spreads through contact with the Mastomy’s rat or an infected human being. The virus is stored in the urine and faeces of these rats. An infected person will spread the virus through their body fluids (blood, faeces and urine).
However, the risk of person-to-person transmission of Lassa fever is low compared to Ebola. In fact, no person-to-person transmission has been reported outside West Africa.
The Lassa fever virus can also spread through the air when you inhale aerosols from the Mastomy’s rat excretion, or materials infected with the virus.

Dry weather conditions enable the spread of the virus and this explains why outbreaks are common between December and April.
According to the Nigerian Centre for Diseases Control (NCDC), Lassa fever has been confirmed in 23 states including Abuja. Ondo State has the highest number of cases at 98. The high number in Ondo may have been influenced by the presence of a free treatment centre.
Diagnosis and Treatment
“Any febrile illness that does not respond to anti-malaria and antibiotics after 48 hours, could be Lassa fever.”
The early signs of Lassa fever are identical to that seen in typhoid and malaria. However, a person infected with the Lassa virus will also have: chest pain, back pain, ringing ears and facial swelling due to loss of fluid from blood vessels.
If you feel unwell and are having any of the symptoms, it is important you go for proper diagnosis and initiate treatment early to increase chances of survival.
Currently, there are a number of Lassa fever diagnostic centres in Nigeria, among them are the three Emergency Operations Centres: the Irrua Specialist Teaching Hospital (Edo State), the Federal Medical Center, Owo (Ondo State) and the Federal Teaching Hospital, Abakiliki (Ebonyi State).
Ribavirin given intravenously during the early stages of the illness is the only recognised treatment for Lassa fever at the moment. In the only study to evaluate the use of Ribavirin, it was found to reduce mortality from 50 per cent – 5 per cent.
Current Situation
“National fatality rate has dropped to below 20%. This means that of the 365 Lassa fever cases in 2020, up to 318 will survive the disease.”
Nigeria has collaborated with both local and international bodies to tackle the disease. However, it cannot be denied that the international community has been relatively silent about this disease spreading through West Africa.
During the severe 2018 Lassa outbreak in Nigeria, there were 633 confirmed cases of Lassa fever and 171 deaths. But Western media preferred to channel their attention to a concurrent Ebola outbreak in Congo which had a similar 600+ cases.
Regardless, there has been a consistent improvement in the handling of Lassa fever cases and behind the scenes are spirited health professionals and passionate volunteers who have risen to the challenge against all odds.
As a result of poor control movement in Nigeria, the spread of the disease has not been properly managed. Even though we now have more cases of the disease, only a small percentage die from the disease. National fatality rate has dropped to below 20 per cent. This means that of the 365 Lassa fever cases in 2020, up to 318 will survive the disease.
Response
“These colleagues are not just government workers because this is not their usual routine. They volunteered to be part of the Emergency Operations Centre and they work even in the face of panic and limited resource.”
- Dr Ahmed Adeagbo Liaso
(Chief Medical Director of FMC Owo)
Since the inspiring story of Sierra Leone’s Aniru Conteh, numerous stories have emerged of resilient healthcare workers who have put themselves at the forefront of the fight against Lassa fever. One of them is Mrs Martha Okonofua, whose story was first published by the Nigeria Health Watch.
Mrs Martha is the matron at the Lassa fever Isolation Ward of the Irrua Specialist Teaching Hospital, Edo State and has been directly involved in managing 200+ Lassa fever patients.

The Irrua Specialist Teaching Hospital has a long standing partnership with the Bernhard-Nocht Institute of Tropical Medicine, Germany and currently leads all local and global researches on Lassa fever.
The Foundation for Innovative New Diagnostics (FIND) is working on a project to improve the response to annual Lassa fever outbreaks in Nigeria through the development of new diagnostics and laboratory strengthening initiatives. This project is in partnership with NCDC and WHO and will be executed at the Irrua Specialist Teaching Hospital.
In 2017, with the help of the government and the Alliance for International Medical Action (ALIMA), a 38-bed capacity Lassa fever Isolation ward was established in FMC Owo, Ondo State.
One of the biggest achievements of the Nigeria Centre for Disease Control (NCDC) was the inclusion of colleagues from the Agricultural and Environmental sector to the Rapid Response Teams (RRTs). This will widen knowledge of environmental and zoonotic factors which are important to control the spread of Lassa fever.
At the moment, there are no approved Lassa fever vaccines but according to the CEO of the NCDC Dr Chikwe Ihekweazu, plans are in place to begin clinical trials for available vaccines in Nigeria.
The three Emergency Operations Centres are not enough to manage patients during outbreaks. It is crucial that more centres are set up in every region of the country. This will not only support early treatment but it will help reduce the unnecessary spread of the virus.
Precautions
“Primary transmission of the Lassa virus from its host to humans can be prevented by avoiding contact with Mastomys rodents, especially in the regions where outbreaks occur.”
No one in Nigeria is safe from this virus and if you fail to apply precautions you might be the next victim of the disease. To protect yourself from the disease you have to ensure proper sanitation; don’t handle rats or any other rodent with your bare hands; store foodstuffs in containers with well-fitting lids.
To prevent human-to-human transmission: avoid crowded areas; don’t travel to areas where the virus is prevalent; preferably wear clothes that do not expose your skin to avoid direct contact with other people’s body fluids.
Nigerians have not yet shown the same level of concern for this year’s Lassa fever outbreak like they did during the previous years’ outbreaks. The reduced fatality rate and discovery of an effective treatment might have contributed but Lassa fever leaves harrowing post-treatment effects (like deafness) on survivors. In the end, the prevention is still better than the cure.











good
Humans dying from infectious diseases worldwide should not matter to anyone in any case.Cities, airports, railway stations also vehicles like trains, aeroplanes should get inundated or submerged underwater by the year 2030. There is no need for ICMR, UN and WHO to address these situations because all these dreadful incidents will self heal our Planet Earth by 111%. Governments, Courts and citizens should be fully aware of the fact that man made things are a total burden to mother nature.
Im obliged for the blog.Much thanks again. Want more.
buy prescription drugs online without: https://genericwdp.com/ india pharmacy mail order
tadalafil generic: http://tadalafilonline20.com/ tadalafil daily use