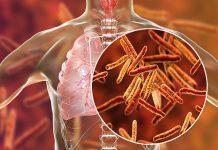
HIV (human immunodeficiency virus) is a virus that attacks the immune system, the body’s natural defence system. Without a strong immune system, the body has trouble fighting off disease. Both the virus and the infection it causes are called HIV.
White blood cells are an important part of the immune system. HIV invades and destroys certain white blood cells called CD4+ cells. If too many CD4+ cells are destroyed, the body can no longer defend itself against infection.
The last stage of HIV infection is AIDS (acquired immunodeficiency syndrome). People with AIDS have a low number of CD4+ cells and get infections or cancers that rarely occur in healthy people. These can be deadly.
But having HIV does not mean you have AIDS. If HIV is diagnosed before it becomes AIDS, medicines can slow or stop the damage to the immune system. With treatment, many people with HIV are able to live long and active lives.
Causes of HIV
HIV infection is caused by the human immunodeficiency virus. You can get HIV from contact with infected blood, semen, or vaginal fluids. Most people get the virus by having unprotected sex with someone who has HIV. Another common way of getting the virus is by sharing drug needles with someone who is infected with HIV.
The virus can also be passed from a mother to her baby during pregnancy, birth, or breast-feeding.
HIV doesn’t survive well outside the body. So it cannot be spread by casual contact such as kissing or sharing drinking glasses with an infected person.
Symptoms of HIV
HIV may not cause symptoms early on. People who do have symptoms may mistake them for the flu or mononucleosis. Common early symptoms include:
· Fever
· Sore throat
· Headache
· Muscle aches and joint pain
· Swollen glands (swollen lymph nodes)
· Skin rash
Symptoms may appear from a few days to several weeks after a person is first infected. The early symptoms usually go away within 2 to 3 weeks.
After the early symptoms go away, an infected person may not have symptoms again for many years. Without treatment, the virus continues to grow in the body and attack the immune system. After a certain point, symptoms reappear and then remain. These symptoms usually include:
· Swollen lymph nodes
· Extreme tiredness
· Weight loss
· Fever
· Night sweats
A doctor may suspect HIV if these symptoms last and no other cause can be found. Treatment usually keeps the virus under control and helps the immune system stay healthy.
Diagnosis of HIV
There are tests that detect HIV antibodies in urine, fluid from the mouth (oral fluid), or blood. If a test on urine or oral fluid shows that you are infected with HIV, you will probably need a blood test to confirm the results. If you have been exposed to HIV, your immune system will make antibodies to try to destroy the virus. Blood tests can find these antibodies in your blood.
Most doctors use two blood tests, called the ELISA and the Western blot assay. If the first ELISA is positive (meaning that HIV antibodies are found), the blood sample is tested again. If the second test is positive, a Western blot will be done to be sure.
It may take as long as 6 months for HIV antibodies to show up in a blood sample. If you think you have been exposed to HIV but you test negative for it, get tested again. Tests at 6, 12, and 24 weeks can be done to be sure you are not infected.
Meanwhile, take steps to prevent the spread of the virus. If you are infected, you can still pass HIV to another person during this time.
Some people are afraid to be tested for HIV. But if there is any chance you could be infected, it is very important to find out. HIV can be treated. Getting early treatment can slow down the virus and help you stay healthy. And you need to know if you are infected so you can prevent spreading the infection to other people.
You can get HIV testing in most doctors’ offices, public health clinics, hospitals, and Planned Parenthood clinics. You can also buy a home HIV test kit in a drugstore or by mail order.
Statistics on HIV/AIDS in Nigeria
Information available from the National Agency for the Control of AIDS (NACA) puts HIV prevalence among the Nigerian population at 3.6 per cent.
National median prevalence among pregnant women is 4.1 per cent.
About 3.1 million people are living with HIV in Nigeria.
About 300,000 new infections occur annually with people aged 15–24 contributing 60 per cent of the infections.
1.5 million People living with HIV require ARVs using the new WHO guidelines.
Only 30 per cent of people living with HIV who need antiretroviral (ARVs) have access to it.
Less than 30 per cent of pregnant women have access to PMTCT services.
Women, Girls and HIV
HIV is the leading cause of death and disease among women of reproductive age (15 – 49 years).
In sub- Saharan African, 60 per cent of the people living with HIV is female (while women make up 50 per cent of the global epidemic).
In Nigeria, prevalence among young women aged 15–24 years is estimated to be three times higher than among men of the same age.
Females constitute 58 per cent (about 1.72 million) of persons living with HIV in Nigeria.
Each year, 55 per cent of AIDS deaths occur among women and girls.
Treatment of HIV
The standard treatment for HIV is a combination of medicines called highly active antiretroviral therapy (HAART). Antiretroviral medicines slow the rate at which the virus multiplies. Taking these medicines can reduce the amount of virus in your body and help you stay healthy.
It may not be easy to decide the best time to start treatment. There are pros and cons to starting HAART before your CD4+ cell count gets too low. Discuss these with your doctor so you understand your choices.
To monitor the HIV infection and its effect on your immune system, a doctor will do two tests:
· Viral load, which shows the amount of virus in your blood;
· CD4+ cell count, which shows how well your immune system is working.
If you have no symptoms and your CD4+ cell count is at a healthy level, you may not need treatment yet. Your doctor will repeat the tests on a regular basis to see how you are doing. If you have symptoms or some other health problems, you should start treatment, whatever your CD4+ count is.
After you start treatment, it is important to take your medicines exactly as directed by your doctor. When treatment doesn’t work, it is often because HIV has become resistant to the medicine. This can happen if you don’t take your medicines correctly. Ask your doctor if you have questions about your treatment.
Treatment has become much easier to follow over the past few years. New combination medicines include two or three different medicines in one pill. Many people with HIV get the treatment they need by taking just one or two pills a day.
Caution during treatment
· Don’t smoke. People with HIV are more likely to have a heart attack or get lung cancer.
· Eat a healthy, balanced diet to keep your immune system strong.
· Get regular exercise to reduce stress and improve the quality of your life.
· Don’t use illegal drugs, and limit your use of alcohol.
· Learn all you can about HIV so you can take an active role in your treatment. Your doctor can help you understand HIV and how best to treat it. Also, consider joining an HIV support group. Support groups can be a great place to share information and emotions about HIV infection.
Prevention of HIV
HIV can be spread by people whether they know they are infected or not. To protect yourself and others:
· Practice safe sex. Use a condom every time you have sex (including oral sex) until you are sure you and your partner are not infected with HIV or other sexually transmitted infection (STI).
· Don’t have more than one sex partner at a time. The safest sex is with one partner who has sex only with you.
· Talk to your partner before you have sex the first time. Find out if he or she is at risk for HIV. Get tested together and retested 6 months later. Use condoms in the meantime.
· Don’t drink a lot of alcohol or use illegal drugs before sex. You might let down your guard and not practice safe sex.
· Don’t share personal items, such as toothbrushes or razors.
· Never share needles or syringes with anyone.
What are Sexually Transmitted Diseases?
Sexually transmitted diseases, commonly called STDs, are diseases that are spread by having sex with someone who has an STD. You can get a sexually transmitted disease from sexual activity that involves the mouth, anus, vagina, or penis.
Types of STDs
· Genital herpes
· Human papilloma virus/genital warts
· Hepatitis B
· Chlamydia
· Syphilis
· Gonorrhoea (“clap”)
Chlamydia
Chlamydia is the most common bacterial sexually transmitted disease (STD) in the U.S. alone. Scientists believe it’s twice as common as gonorrhoea and 30 times as common as syphilis. The good news is that chlamydia is easily cured by antibiotics. The bad news is that 50 per cent of women who contract the disease don’t know they are infected and 30 per cent develop serious complications such as damage to the fallopian tubes (the tubes that connect the ovaries to the uterus)
Symptoms of Chlamydia
Often, chlamydia will present no symptoms. When symptoms are present, common ones include (in men): A clear or whitish yellow discharge from the tip of the penis; a frequent urge to urinate or a burning sensation while urinating; redness at the tip of the penis; (in women): mild discomfort that you may mistake for menstrual cramps; vaginal discharge that may have a bad smell; bleeding between periods; painful periods; pain when having sex ; itching or burning in or around the affected part.
Diagnosis of Chlamydia
There are a few different tests your doctor can use to diagnose chlamydia. He or she will probably use a swab to take a sample from the urethra in men or from the cervix in women and then will send the specimen to a laboratory to be analysed. There are also other tests which check a urine sample for the presence of the bacteria.
Treatment of Chlamydia
If you have chlamydia, your doctor will prescribe oral antibiotics, usually azithromycin (Zithromax) or doxycycline. Your doctor will also recommend your partner(s) be treated as well to prevent reinfection and further spread of the disease.
With treatment, the infection should clear up in about a week or two. It is important to finish all of your antibiotics even if you feel better.
Women with severe chlamydia infection may require hospitalisation, intravenous antibiotics (medicine given through a vein), and pain medicine.
After taking antibiotics, people should be re-tested to be sure the infection is cured. This is particularly important if you are unsure that your partner(s) obtained treatment. Do not have sex until you are sure both you and your partner no longer have the disease.
Genital Herpes
Herpes is caused by the herpes simplex virus (HSV). HSV-type 1 commonly causes fever blisters on the mouth or face (oral herpes), while HSV-type 2 typically affects the genital area (genital herpes). However, both viral types can cause either genital or oral infections. Most of the time, HSV-1 and HSV-2 are inactive, or “silent,” and cause no symptoms, but some infected people have “outbreaks” of blisters and ulcers. Once infected with HSV, people remain infected for life.
Transmission of Genital Herpes
HSV-1 and HSV-2 are transmitted through direct contact, including kissing, sexual contact (vaginal, oral, or anal sex), or skin-to-skin contact.
Genital herpes can be transmitted with or without the presence of sores or other symptoms. It often is transmitted by people who are unaware that they are infected, or by people who do not recognize that their infection can be transmitted even when they have no symptoms.
Treatment of Herpes
There is no treatment that can cure herpes, but antiviral medications can shorten and prevent outbreaks for whatever period of time the person takes the medication.
Prevention of Herpes
The consistent and correct use of latex condoms is the best protection. However, condoms do not provide complete protection, because a herpes lesion may not be covered by the condom and viral shedding may occur. If you or your partner has genital herpes, it is best to abstain from sex when symptoms are present, and to use latex condoms between outbreaks.
Genital Warts and HPV
Warts are caused by viruses and can appear anywhere on the body. Those that show up in the genital area are caused by the human papilloma virus, commonly called HPV, and are easily transmitted by sexual contact.
Description of Genital Warts
Genital warts look like small flesh-coloured, pink or red growths in or around the sex organs. The warts may look similar to the small parts of a cauliflower or they may be very tiny and difficult to see. They often appear in clusters of three or four, and may grow and spread rapidly. They usually are not painful, although they may cause mild pain, bleeding, and itching.
Genital Wart Symptoms
Like many STDs, HPV does not always have visible symptoms. But when symptoms do occur, warts may be seen around the genital area. In women, warts can develop on the outside and inside of the vagina, on the cervix (the opening to the uterus), or around the anus. In men, they may be seen on the tip of the penis, the shaft of the penis, on the scrotum, or around the anus. Genital warts also can develop in the mouth or throat of a person who has had oral sex with an infected person.
Genital Wart Diagnosis
Your doctor may perform the following tests to check for genital warts and/or related STDs:
· An examination of visible growths to see if they look like genital warts
· Application of a mild acetic acid (vinegar) solution to highlight less visible growths
· A complete pelvic exam and Pap smear (for women)
· A specialized test for HPV, collected in a way similar to a Pap smear
· Biopsy of cervical tissue to make sure there are no abnormal cells that could develop into HPV-related cervical cancer; a cervical biopsy involves taking a small sample of tissue from the cervix and examining it under a microscope.
· Examination of the rectum
Sometimes female patients are referred to a gynaecologist (a doctor who specialises in female reproductive health) for further testing and biopsy.
Hepatitis B
Hepatitis B is a serious disease caused by the hepatitis B virus (HBV). Infection with this virus can cause scarring of the liver, liver failure, liver cancer, and even death.
Hepatitis B is spread in infected blood and other bodily fluids such as semen and vaginal secretions. It is spread in the same way that the virus that causes AIDS (HIV) is spread but hepatitis B is 100 times more infectious.
Signs and Symptoms of Hepatitis B
Symptoms of acute infection (when a person is first infected with hepatitis) include:
· Jaundice (yellowing of the skin or whites of the eyes and/or a brownish or orange tint to the urine)
· Unusually light coloured stool
· Unexplained fatigue that persists for weeks or months
· Flu-like symptoms such as fever, loss of appetite, nausea, and vomiting
· Abdominal pain
Often, symptoms occur one to six months after exposure. An estimated 30 per cent of those infected do not have any symptoms at all.
People with chronic active hepatitis experience similar symptoms, but their fatigue is much more severe, and they can have confusion or disorientation.
Hepatitis B Diagnosis
If your doctor suspects that you may have hepatitis B, he or she will perform a complete physical exam and order blood tests to look at the function of your liver. Hepatitis B is confirmed with blood tests that detect the virus.
If your disease becomes chronic, liver biopsies (tissue samples) may be obtained to detect the severity of the disease.
Treatment of Hepatitis B
If you get to a doctor shortly after the exposure, you’ll often receive immediate immunization with the first in a series of three shots with the hepatitis B vaccination and a shot to boost the immune system to fight off the infection.
Also, take extra care of your liver! Now is not the time to drink alcohol, or take Tylenol (acetaminophen) because they can harm the liver. Check with your doctor before taking any other medications, herbal remedies, or supplements as some of them can worsen liver damage.
If your hepatitis persists beyond six months and is active (chronic active hepatitis), your doctor may prescribe much more aggressive treatment. If it’s chronic but not active, your doctor may just watch you closely.
People with chronic active hepatitis are treated with a combination of drugs like the following:
·Interferon.
The immune system boosting medicine interferon is injected daily, several times a week, or weekly for up to a year. Interferon does have some undesirable side effects, including: fatigue, depression, and loss of appetite and it can lower the number of white blood cells. There are two types of interferon: interferon-alfa (Intron) and peginterferon alfa (Pegasys).
·Epivir.
Another drug often given in combination with interferon is lamivudine (Epivir). This drug is taken orally once a day. Usually, this drug is well tolerated, but it can cause a worsening of liver functioning in rare instances.
·Hepsera.
This drug is taken by pill once a day and works well in people whose disease doesn’t respond to Epivir. It can cause kidney problems especially in people that already have kidney disease, but it can occur in anyone. ·
Baraclude.
This drug is taken by pill daily and studies are showing it may be one of the most effective antiviral drugs available for hepatitis B.
Viread (Tenofovir):
A once daily pill. It is also used to treat HIV and is used in patients who have both HIV and Hepatitis B. It can also be used as a single agent for Hepatitis B.
Hepatitis B in pregnancy
A pregnant woman can spread the hepatitis B virus to her baby at the time of birth. (It is unlikely that an infected woman will spread the virus to her baby during pregnancy.)
Many babies infected with hepatitis B develop long-term liver problems. All newborn babies should be given the vaccine for hepatitis at birth and two additional booster injections during their first year of life.
Prevention of Hepatitis B
The best ways to try and avoid becoming infected with hepatitis B include:
· Get vaccinated (if you have not already been infected).
· Use condoms every time you have sex.
· Wear gloves when touching or cleaning up body secretions on personal items, such as bandages/band aids, tampons, and linens.
· Cover all open cuts or wounds.
· Do not share razors, toothbrushes, manicuring tools, or pierced jewellery with anyone.
· Do not share chewing gum or pre-chew food for a baby.
· Make certain that any needles for drugs, piercing, or tattooing are properly sterilised.
· Clean areas with blood on them with one part household bleach and 10 parts water.
Syphilis
Syphilis is a highly contagious disease spread primarily by sexual activity, including oral and anal sex. Occasionally, the disease can be passed to another person through prolonged kissing or close bodily contact. Although this disease is spread from sores, the vast majority of those sores go unrecognized. The infected person is often unaware of the disease and unknowingly passes it on to his or her sexual partner.
Pregnant women with the disease can spread it to their baby. This disease, called congenital syphilis, can cause abnormalities or even death to the child.
Syphilis cannot be spread by toilet seats, door knobs, swimming pools, hot tubs, bath tubs, shared clothing, or eating utensils.
Syphilis is caused by the bacteria Treponema pallidum.
How Is Syphilis Treated?
If you’ve been infected with syphilis for less than a year, a single dose of penicillin is usually enough to destroy the infection. For those allergic to penicillin, tetracycline or doxycycline can be given instead. If you are in a later stage of disease, more doses will be needed.
People who are being treated for syphilis must abstain from sexual contact until the infection is completely gone. Sexual partners of people with syphilis should be tested and, if necessary, treated.
Gonorrhoea
Also called the “clap” or “drip,” gonorrhoea is a contagious disease transmitted most often through sexual contact with an infected person. Gonorrhoea may also be spread by contact with infected bodily fluids, so that a mother could pass on the infection to her newborn during childbirth. Both men and women can get gonorrhoea. The infection is easily spread and occurs most often in people who have many sex partners.
What Causes Gonorrhoea?
Gonorrhoea is caused by Neisseria gonorrhoea, a bacterium that can grow and multiply easily in mucus membranes of the body. Gonorrhoea bacteria can grow in the warm, moist areas of the reproductive tract, including the cervix (opening to the womb), uterus (womb), and fallopian tubes (egg canals) in women, and in the urethra (the tube that carries urine from the bladder to outside the body) in women and men. The bacteria can also grow in the mouth, throat, and anus.
Gonorrhoea symptoms in women
· Greenish yellow or whitish discharge from the vagina
· Lower abdominal or pelvic pain
· Burning when urinating
· Conjunctivitis (red, itchy eyes)
· Bleeding between periods
· Spotting after intercourse
· Swelling of the vulva (vulvitis)
· Burning in the throat (due to oral sex)
· Swollen glands in the throat (due to oral sex)
In some women, symptoms are so mild that they escape unnoticed. Many women with gonorrhoea discharge think they have a yeast infection and self-treat with over-the-counter yeast infection drug. Because vaginal discharge can be a sign of a number of different problems, it is best to always seek the advice of a doctor to ensure proper diagnosis and treatment.
Gonorrhoea symptoms in men
· Greenish yellow or whitish discharge from the penis
· Burning when urinating
· Burning in the throat (due to oral sex)
· Painful or swollen testicles
· Swollen glands in the throat (due to oral sex)
In men, symptoms usually appear two to 14 days after infection.
How Is Gonorrhoea Diagnosed?
To diagnose gonorrhoea, your doctor will use a swab to take a sample of fluid from the urethra in men or from the cervix in women. The specimen will then be sent to a lab to be analysed. You also may be given a throat or anal culture to see if the infection is in your throat or anus. There are other tests which check a urine sample for the presence of the bacteria. You may need to wait for several days for your tests to come back from the lab.
Gonorrhoea and chlamydia, another common sexually transmitted disease, often occur together, so you may be tested and treated for both.
Can Gonorrhoea Be Cured?
Yes. Gonorrhoea can be treated and cured.
How Is Gonorrhoea Treated?
To cure a gonorrhoea infection, your doctor will give you either an oral or injectable antibiotic. Your partner should also be treated at the same time to prevent reinfection and further spread of the disease.
It is important to take all of your antibiotics even if you feel better. Also, never take someone else’s medication to treat your illness. By doing so, you may make the infection more difficult to treat. In addition, tell anyone you have had sex with recently that you are infected. This is important because gonorrhoea may have no symptoms. Women, especially, may not have symptoms and may not seek testing or treatment unless alerted by their sex partners.
Don’t have sex until you have completed taking all of your medicine. Always use condoms when having sex.
What Happens if I Don’t Treat Gonorrhoea?
Untreated gonorrhoea can cause serious and permanent problems in both women and men. In women, if left untreated, the infection can cause pelvic inflammatory disease, which may damage the fallopian tubes (the tubes connecting the ovaries to the uterus) or even lead to infertility, and untreated gonorrhoea infection could increase the risk of ectopic pregnancy (when the fertilised egg implants and develops outside the uterus), a dangerous condition for both the mother and baby.
In men, gonorrhoea can cause epididymitis, a painful condition of the testicles that can sometimes lead to infertility if left untreated. Without prompt treatment, gonorrhoea can also affect the prostate and can lead to scarring inside the urethra, making urination difficult.
Gonorrhoea can spread to the blood or joints. This condition can be life-threatening. Also, people with gonorrhoea can more easily contract HIV, the virus that causes AIDS. People with HIV infection and gonorrhoea are more likely than people with HIV infection alone to transmit HIV to someone else.
Prevention of Gonorrhoea Infection
To reduce your risk of gonorrhoea infection:
· Use condoms correctly every time you have sex.
· Limit the number of sex partners, and do not go back and forth between partners.
· Practice sexual abstinence, or limit sexual contact to one uninfected partner.
· If you think you are infected, avoid sexual contact and see a doctor.
Any genital symptoms such as discharge or burning during urination or an unusual sore or rash should be a signal to stop having sex and to consult a doctor immediately. If you are told you have gonorrhoea or any other STD and receive treatment, you should notify all of your recent sex partners so that they can see a doctor and be treated.
Source:WebMD Medical Reference